M.D. Vojtěch Hanulík, Ph.D. is board-certified doctor in microbiology and dermatovenerology, his speciality are antibiotic-resistant bacteria and skin conditions such as psoriasis and atopic eczema. His work goes beyond the confines of laboratory, as he is actively involved in clinical practice, antibiotic therapy and complex care of patients with dermatological problems. His work is a combination of scientific approach and direct patient care.
Microbiology in Central Europe is still primarily laboratory work, but it is increasingly shifting towards clinical practice. This involves consultations with colleagues in hospitals, recommending and monitoring antibiotic therapy for individual patients, as well as overseeing overall antibiotic consumption within hospital facilities.
Dermatology is a clinical field that encompasses several areas. A significant part of the work involves skin diseases such as psoriasis, atopic eczema, and skin allergies. Additionally, we treat skin conditions resulting from other diseases, such as rheumatic or oncological disorders. We are involved in the prevention, diagnosis, and therapy of skin tumors, caring for both acute and chronic skin defects. Venereology, which includes sexually transmitted diseases, is also part of our scope of practice.
You originally studied microbiology, and then you also worked with those tiny organisms. What attracted you to that field, and why did you later decide to pursue dermatovenereology?
Vojtěch: Microbiology, especially highly infectious diseases, fascinated me ever since I read Preston’s “The Hot Zone” during high school. Working in the laboratory and peering through the microscope always brought me great joy. However, an opportunity arose to change my field, and I seized it. It turned out to be one of the best decisions of my life. I do dermatology truly for my own pleasure. In microbiology, I missed direct contact with patients.
In dermatology, as I mentioned before, there are numerous opportunities for specialization. I particularly enjoy the option of combining this field with surgery, which I have a great fondness for. Moreover, it often intersects with microbiology in many cases. We frequently deal with skin issues caused by viral or bacterial agents, and allergic reactions to antibiotics manifest as regular skin problems. Venereology is purely infectious in nature. Even in the treatment of chronic wounds, a doctor must be able to decide whether the wound is colonized by bacteria or if it has progressed to an infection requiring systemic antibiotic therapy. This can be quite an art at times. Thanks to my knowledge in microbiology, I believe I have a more comprehensive view of the relationship between humans and microorganisms.
Are you the type of doctor who has learned something and now just relies on old practices, or do you continue to educate yourself beyond the scope of your profession?
Vojtěch: I do struggle quite a bit with my inherent laziness, and it’s true that routine matters are, in a way, a form of relaxation for me. But certainly, a doctor must continually educate themselves.
I admit that I have my classic “well-tried methods” when it comes to the strategy of treatment and therapy for certain diseases in general. It’s a foundation proven by experience – a combination and approach that usually works well for a given problem. If it fails, it can be adjusted individually. At that point, one must engage the mind, consult the internet, or open a book.
Staying informed and delivering the best that contemporary medicine can offer to the patient is, in my opinion, still crucial. However, there are areas in which I have foregone further education and expanding my horizons.
Does your profession have an impact on you? By that, I mean, when you know what causes certain skin diseases, such as bacteria, viruses, or substances contained in lotions or cosmetics… do you avoid them?
Vojtěch: I personally don’t regularly use dermocosmetics. In this aspect, I’m probably an average guy. I hold the opinion that circumstances and advertisements convince us of an almost anxious care for the skin, whether for health or at least for beauty. The truth, however, is that the normal skin of a generally healthy person doesn’t require specific care. In fact, excessive use of soaps in washing can harm the skin rather than benefit it. Healthy skin is capable of creating a resilient protective layer on its own, including natural oils and body-specific bacteria. Washing too frequently can disrupt this protective layer and lead to skin diseases. Those particularly susceptible are individuals with atopic conditions, where the skin’s protective function is naturally weakened. Of course, this doesn’t mean neglecting personal hygiene. I had a patient who was an aerobics instructor. According to her, she was either sweating or under the shower. Washing multiple times a day with shower gel, she constantly suffered from dry and irritated skin. A simple adjustment to her routine – rinsing with water after exercise, using soap on the skin roughly every other day, and occasionally moisturizing the skin at night – resolved her issues.
What do patients most commonly come to you for?
Vojtěch: I have a general practice, so the range of conditions I encounter is quite broad. However, the most common issues include atopic eczema, psoriasis, venous leg ulcers, and tumor changes on the skin. I frequently address fungal infections of the skin and nails, viral warts, scabies, hair loss, contact allergies, eczemas, and among acute conditions, erysipelas, shingles, or hives.
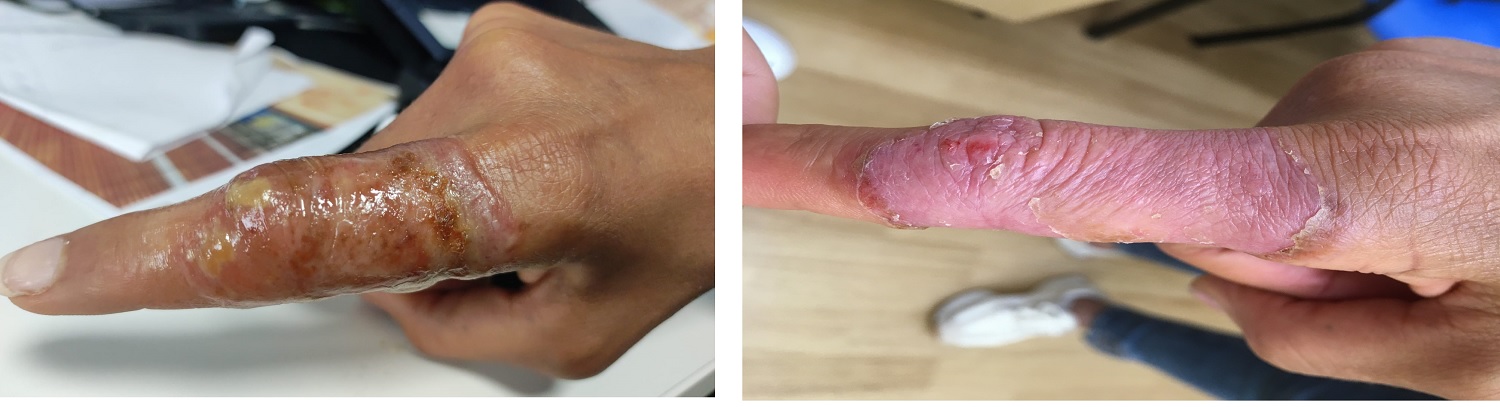
Picture source: Vojtěch Hanulík; Fungal infection before and after treatment
I observe how many people around me have some inflammatory skin conditions (eczema, atopic eczema, dermatitis…). Could you please briefly describe what these terms mean and what the differences are?
Vojtěch: Even experts often confuse these terms, and it’s often a matter of semantics. Dermatitis, in simplified terms, refers to inflammatory skin conditions where an allergic cause is not presumed. Eczemas are essentially the same inflammatory skin reactions, but the cause is linked to some allergen. The clinical difference in symptoms can be very similar in both groups of conditions. There is also frequent confusion between these terms, and one might encounter both atopic eczema and atopic dermatitis.
When I ask these individuals or parents of children with eczema, for example, what triggers it, I don’t receive the same answers. So, what about skin inflammations, and why do so many people have them?
Vojtěch: Atopy is a predisposition to an inadequate skin reaction, partially innate and linked within families. I explain it to my patients as follows: the skin of an atopic person is like a poorly constructed wall. If the wall of a house is to withstand common weather conditions, it must be built with the right bricks that are properly fired. The proper mortar must be used, with the correct ratio of water, sand, lime, cement, etc. If not, the wall cannot withstand the effects of rain, sun, and wind and gradually deteriorates. Similarly, with atopic skin, some structural components are naturally lacking, or conversely, there are excess enzymes that rapidly break down this wall. We usually don’t identify specific molecules, but with proper care, we can improve our skin’s barrier, and by applying the necessary substances, we can sometimes restore its protective function permanently.
Atopy is complicated by the fact that it is also associated with an inadequate immune response. Therefore, the skin reacts more quickly to inflammation due to stress, dryness, bacterial overgrowth, and other factors.
We know quite a bit about the triggering factors of atopic dermatitis, and each atopic individual can observe over time what worsens or improves their symptoms. However, we don’t know much about the actual cause. Personally, I find the so-called hygiene hypothesis very interesting. It establishes a connection between the lower prevalence of human parasites in the population and the increasing incidence of autoimmune diseases in recent decades. Over two or three generations, we haven’t switched off our immunity against parasites, and it often contributes to the development or worsening of autoimmune and inflammatory diseases. However, it’s still a theory, but as a microbiologist, I see a great deal of logic in it. As usual, it doesn’t explain everything.
According to about 10 interviews I conducted with people suffering from ATOPIC eczema, there was consensus that doctors immediately prescribed corticosteroid ointments, even to very young children, without adequately explaining the issues related to the condition and the application of corticoid preparations. What does current science recommend, and what is your advice based on your practice?
Vojtěch: This is quite a fundamental topic. On one hand, we encounter strict opponents of corticoids; on the other hand, contemporary medicine essentially has nothing better and more accessible for quickly stopping skin inflammation. There are immune modulators with a similar effect, but they are not as fast and reliable (I’m referring to products with tacrolimus and pimecrolimus – Protopic, Elidel). Many people come to the clinic and say they don’t want external corticoids because their symptoms return after using them, sometimes even worse. It’s a delicate question, especially when it comes to small children.
Personally, I wouldn’t do without corticoid therapy, but it’s crucial to know when and how to use it. The patient should be thoroughly and repeatedly educated about it.
When I get to the essence, corticoids help us calm skin inflammation. After calming, and often during corticoid therapy, it is equally important to use appropriate ointments. Refer to what I mentioned earlier about poorly constructed walls. After calming, we transition to so-called interval therapy, meaning we intensely apply suitable creams and ointments and occasionally add a corticoid preparation. We try to prolong the interval between corticoid applications as much as possible. On the other hand, if the inflammation worsens, I don’t hesitate to use corticoids and suppress the inflammation symptoms at the onset.
For children and on facial skin, we use different corticoids than on thicker skin, and every dermatologist should be well-educated and able to advise on this. The key is to clearly convey this information to patients.
A completely different approach is offered by physical therapy with the excimer laser. It operates with a wavelength of 308 nm, which destroys inflammatory cells at the sites of manifestations. The effect is equivalent to the use of external corticoids without the risk of side effects. It can be used for a wide range of skin diseases (psoriasis, atopic eczema, alopecia, vitiligo, pustular dermatosis, treatment of fungal nail infections, and many others). The drawback is that most health insurance covers the therapy only for psoriasis manifestations. However, the results here are truly excellent and long-lasting. Not every excimer laser on the market is equally effective, so choosing highly efficient therapy devices is necessary. (Author’s note: it is a laser that removes individual tissue particles by pulsing beams without damaging the surrounding tissue.) Such lasers are practically available in every regional city in the Czech Republic.
When there is any skin injury, such as eczema, scratches, various pimples, allergic reactions, etc., such disruption of the skin allows easier entry of various components further into the body. This can be a problem, especially with the prolonged application of products containing harmful substances. Is it appropriate to apply ointments and creams to damaged skin? What is generally recommended, but not widely known?
Vojtěch: In this case I would probably distinguish between acutely occurring skin defects, such as wounds or abrasions, and chronic conditions, including the mentioned eczemas. If I am consistently applying any product to a chronic condition where an inflammatory reaction is ongoing, there is always a risk of greater penetration of the product’s components into the skin and potential sensitization. However, for acute defects, everyone is likely familiar with some suitable ointment that can promote healing.
As a rule, I stick to established companies that have been dealing with dermocosmetics and the treatment of skin diseases for a long time. These are companies that have their products prepared to minimize irritation and harm, at least that’s my conviction. Nevertheless, everyone has different preferences, and some might find even homemade hemp ointment sufficient.
Moles and skin cancer, you probably encounter that as well, right? Is skin cancer common in the Czech Republic? Can it be effectively treated?
Vojtěch: Skin cancer is very common in the Czech Republic, and the incidence of skin malignancies in the population is on the rise. It is important to distinguish between malignant melanomas and non-melanoma skin cancers. Melanomas, in simplified terms, originate from moles and can occur anywhere on the skin and essentially at any age. Non-melanoma cancers occur mainly in older individuals, especially on skin that has been exposed to sunlight for a long time, often presenting as non-healing skin sores.
Treatment is straightforward in the early stages, where the tumor can be excised under local anesthesia, and the patient is regularly monitored thereafter. In cases of more advanced stages, the therapy is more complex and demanding, typically involving a combination of surgical intervention and subsequent oncological treatment.
Late-stage melanomas have a very poor prognosis, as do advanced non-melanoma skin cancers, especially those located in anatomically unfavorable areas. Therefore, everyone should take advantage of the opportunity to have their moles checked at least once a year.
While it has been mentioned on various websites and publications, can you tell us what to watch out for? When to see a doctor… sometimes moles look quite strange and are not “faulty,” why does this happen at all?
Vojtěch: The primary risk factor for melanoma is repeated sunburn. For the development of non-melanoma skin tumors, the crucial role is played by the cumulative exposure to sunlight throughout one’s life, indicating the intensity of sun exposure. Genetic predisposition is also significant. Families with a higher genetic burden have a greater likelihood of developing skin tumors. Therefore, if any type of skin tumor is present in the family (parent/siblings), regular dermatological examinations are advisable. As I mentioned, every patient can have moles regularly examined preventively. A referral from a general practitioner is not required for an examination by a dermatovenereologist, and patients can schedule an appointment on their own.
Moles are examined with a device called a dermatoscope, which comes in both traditional and digital forms. The traditional dermatoscope is essentially an illuminated magnifying glass used to inspect individual moles. By looking for specific risk features and evaluating them, dermatologists determine whether a mole is suitable for excision or just requires monitoring. The digital dermatoscope performs this process automatically using a computer algorithm. However, it is generally acknowledged that an experienced dermatologist with a traditional dermatoscope is more precise in diagnosing skin tumors than an inexperienced one with a digital dermatoscope. The advantage of the digital dermatoscope lies in its ability to easily store photos of individual lesions and compare any changes over time. There is also a digital dermatoscope combined with a full-body scanner, capable of recognizing changes in moles on the body over longer time intervals. This is useful for patients with a larger number of moles.
A thorough dermatologist, among other things, can be identified by carefully examining moles, looking at the entire body surface, including the scalp, breasts in women, and the soles of the feet and nails. Skin tumors can be hidden in these areas without notice.
Personally, I have a small beauty mark on my face (similar to Cindy Crawford’s 🙂). Is it better to remove it when it is very often exposed to sunlight?
Vojtěch: There must be a reason to remove a mole. If there is suspicion of a malignant process or if the mole is mechanically irritated, it is necessary to gently excise the mole under local anesthesia and have it examined by a pathologist. If the reason is purely aesthetic, the approach is slightly different. There are methods for removal, such as laser or cautery. However, only an experienced dermatologist should indicate this. I would like to caution against the unnecessary removal of moles with lasers. In most cases, a gentle stitched excision or removal of the lesion for examination by a pathologist is preferable. Fractional laser removal usually doesn’t allow for a proper examination of the mole. Moreover, I repeatedly encounter cases where a non-dermatologist removes a mole with a laser, charges a considerable amount of money, and after a few years, a scar starts to grow in the place of the incompletely removed mole. Such a manifestation cannot be reliably assessed by a routine examination, and excision becomes necessary.
In general, it is not true that a mole exposed to sunlight is more prone to the development of melanoma. These factors are not related. Removing such a cosmetic imperfection will replace it with a more or less satisfactory different cosmetic defect. The decision is then more up to the patient.
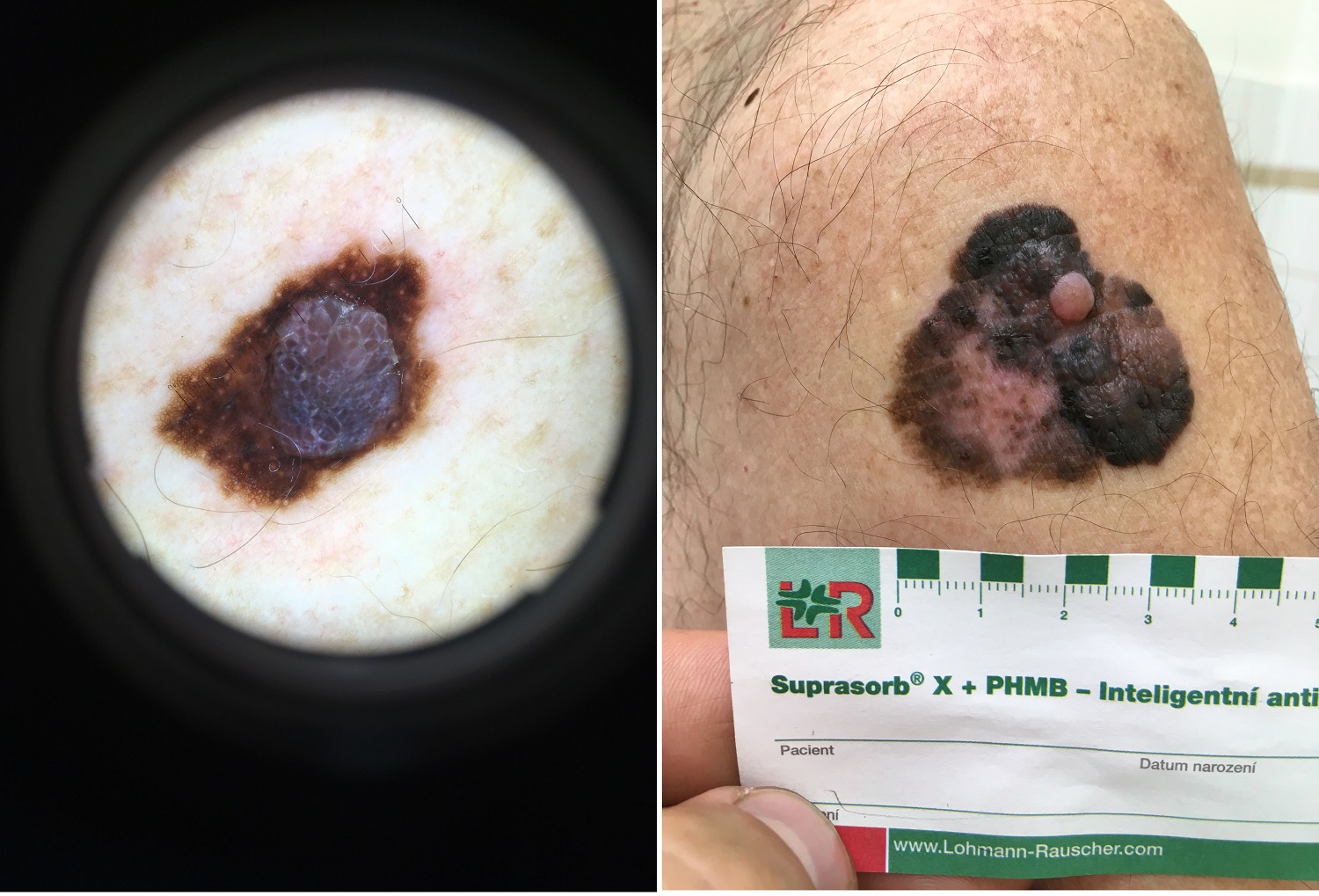
Picture source: Vojtěch Hanulík; Melanoma, malignant melanoma
Are you a fan of sunscreen, or do you prefer recommending light cotton clothing, hats, etc.?
Vojtěch: Certainly, yes. For people who enjoy the sun, it is an ideal way to prevent either skin cancer or early signs of aging. Combining it with a cap or hat is crucial for men who have lost hair on their heads.
From my perspective, it doesn’t matter which type of sunscreen is used. However, I recommend a higher SPF, and most importantly, we must not forget to reapply sunscreen at regular intervals.
And how do you perceive children from the perspective of skin, sun, and lotions ?
Vojtěch: Although neither my wife nor I suffer from atopic eczema, our two children do, albeit in a mild form. Especially in the case of our younger daughter, her skin becomes very dry in the fall. Therefore, I don’t shy away from using creams and lotions on my own children or my pediatric patients. However, I primarily choose simple ointment bases such as Ambiderman, Leniens, or Cutilan. Especially with the first rays of sunshine and during vacations abroad, my wife and I try to protect our children from sunburn. As I mentioned earlier, it is one of the significant risk factors for the development of skin tumors in adulthood and old age.
And it just have to ask 🙂… why is the combination of skin and venereal diseases a specialty?
Vojtěch: I pondered that too. The reason is likely the historically most significant sexually transmitted disease – syphilis, which exhibits characteristic skin manifestations in all stages of the illness. In the early days of modern medicine, the treatment of syphilis by dermatologists probably gave rise to venereology as a distinct medical speciality.
How do you perceive various intimate hygiene products, especially for women but also for men? Generally, gynecologists advise against using various products, but advertisements suggest otherwise. For example, my gynecologist once told me, when I had some issues, that I needed to wash less and, above all, without any specific product, and it helped :). Have you encountered something similar in your practice?
Vojtěch: It is very similar to what I mentioned regarding caring for atopic skin. One should certainly not stink, but washing with soap excessively will sooner or later exhaust the skin’s protective capacity and cause skin problems. In the genital area, this often manifests as yeast infections. Frequently, young boys and men come to me with complaints of reddened glans and itching in the genital area. They shower and claim to wash thoroughly several times a day, which is often the fundamental problem. We provide a soothing cream, discuss lifestyle measures, and within a few days, the issue is usually resolved. The same applies to women. For intimate hygiene, clean water is usually sufficient, and if needed, choosing products specifically designed for intimate hygiene that are gentle on the skin’s protective layers is advisable. Sometimes, less is more.
Thank you very much for your time!


0 Comments